Archive for Nerdview
May 5, 2024 @ 9:06 am· Filed by Mark Liberman under Elephant semifics, Nerdview
In a comment on yesterday's "Software testing day" post, ernie in berkeley offered a nice "QA Engineer walks into a bar" joke, and pointed us to its origin in an old xkcd comic "Exploits of a Mom":
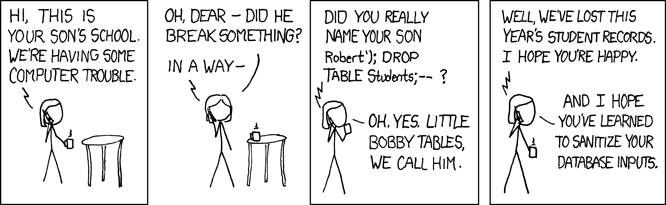
…which in turn reminded me of an old problem, discussed in "Excel invents genes", 8/26/2016:
Read the rest of this entry »
Permalink
August 8, 2022 @ 4:22 am· Filed by Victor Mair under Language and computers, Nerdview
Three years ago, we visited a proposal for "Classical Chinese computing" (12/19/19). The post began thus:
Several colleagues called this article to my attention:
"Programming Language for the ancient Chinese"
Here's the introduction:
文言, or wenyan, is an esoteric programming language that closely follows the grammar and tone of classical Chinese literature. Moreover, the alphabet of wenyan contains only traditional Chinese characters and 「」 quotes, so it is guaranteed to be readable by ancient Chinese people. You too can try it out on the online editor, download a compiler, or view the source code.
The home page then goes through "Syntax", "Compilation", and "Get (Source Code; Online Editor; Reference".
Read the rest of this entry »
Permalink
December 19, 2019 @ 1:44 pm· Filed by Victor Mair under Language and computers, Nerdview
Several colleagues called this article to my attention:
"Programming Language for the ancient Chinese"
Here's the introduction:
文言, or wenyan, is an esoteric programming language that closely follows the grammar and tone of classical Chinese literature. Moreover, the alphabet of wenyan contains only traditional Chinese characters and 「」 quotes, so it is guaranteed to be readable by ancient Chinese people. You too can try it out on the online editor, download a compiler, or view the source code.
The home page then goes through "Syntax", "Compilation", and "Get (Source Code; Online Editor; Reference".
Read the rest of this entry »
Permalink
March 6, 2018 @ 12:51 am· Filed by Neal Goldfarb under blegs, Nerdview, Philosophy of Language, Typography, Usage advice, Writing systems, WTF
In MS Word, buried deep in File|Options|Advanced|Compatibility Options|Layout is the option to check 'Do full justification the way WordPerfect 6.x for Windows does'". If you use full justification, your document will look ugly unless you check that box.
Does that qualify as a form of nerdview?
Permalink
November 18, 2017 @ 9:05 am· Filed by Geoffrey K. Pullum under Language and business, Language and computers, Nerdview, Silliness
This is a screen shot I snapped during a recent attempt to purchase something (can't remember what) on the web:
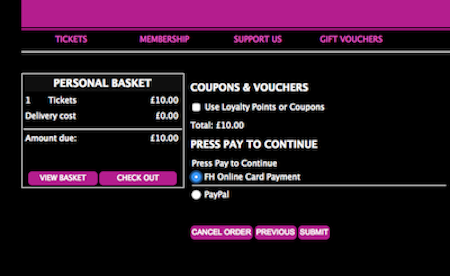
Notice that in order to continue, it tells me (twice) that I have to press "Pay". Can you see any button labeled "Pay" on the screen?
If you are itching to tell me what I should have done, you are missing my point.
Read the rest of this entry »
Permalink
August 30, 2017 @ 11:54 am· Filed by Geoffrey K. Pullum under Nerdview

In various areas of Edinburgh there are signs that say "Peripheral Controlled Zone." What exactly would you do if you encountered one of these signs? What would it mean to you? Not much? That's the hallmark of nerdview.
What is peripheral to what? Who is controlling what? What is peripheral control? Why are you being told this? Nothing becomes clearer as you mull over what it says. They might as well have put up a sign saying "Argle bargle nurff gugga mongmong gooboo wah Mon – Fri 8:30am – 5:30pm."
But worse, if you did know what it meant you would become aware that it could not possibly be relevant to you.
Read the rest of this entry »
Permalink
February 9, 2017 @ 4:43 pm· Filed by Geoffrey K. Pullum under Language and computers, Lost in translation, Nerdview
Steve Politzer-Ahles was trying to change his password on the Hong Kong Polytechnic University system, and found himself confronted with this warning:
You may not use the following attribute values for your password:
puAccNetID
puStaffNo
puUserGivenName
puUserSurname
Attribute values? This is classic nerdview.
Read the rest of this entry »
Permalink
December 18, 2016 @ 8:43 am· Filed by Geoffrey K. Pullum under Nerdview, Psychology of language, Signs
It's good to find a prominently displayed list of local bus routes that you can  consult when you arrive at the train station in a big city that perhaps you do not know.
consult when you arrive at the train station in a big city that perhaps you do not know.
And Sydney Central station in New South Wales, Australia, has exactly that. There is a big board headed "Find your way" at the station. But let's take a closer look at it. See if you can spot the nerdview (pointed out to me by Language Log reader Geoff Dawson).
Read the rest of this entry »
Permalink
September 12, 2016 @ 12:03 am· Filed by Geoffrey K. Pullum under Found in translation, Humor, Intelligibility, Language and travel, Language contact, Languages, Multilingualism, Names, Nerdview, Silliness, This blogging life, Translation, Words words words, World language, WTF
At my hotel here in Brno, Czechia, the shampoo comes in small sachets, manufactured in Düsseldorf, labeled with the word denoting the contents in a long list of suitable European Union languages. I can't tell you which languages they picked, for reasons which will immediately become apparent. Here are the first four:
- Shampoo
- Shampoo
- Shampooing
- Shampoo
Just so you're sure.
Read the rest of this entry »
Permalink
September 5, 2016 @ 9:53 am· Filed by Geoffrey K. Pullum under Nerdview
Hurricane Statement
Issued: 5:25 AM EDT Sep. 5, 2016 – National Weather Service
This product covers southern New England
Northeast wind gusts of 30 to 50 mph expected from 10 am to 8 PM this evening on the South Coast…
Tim Leonard is quite right to point out that when the National Weather Service refers to its storm warning announcement as a "product", that is nerdview.
It is a product only as viewed from within the staff of the NWS, where they would have no function and no jobs if they did not produce such things. For us out here in the weather, it is not a product, it is a warning.
Permalink
September 5, 2016 @ 4:59 am· Filed by Geoffrey K. Pullum under Language and computers, Nerdview
Adam Rosenthal told me in an email recently: 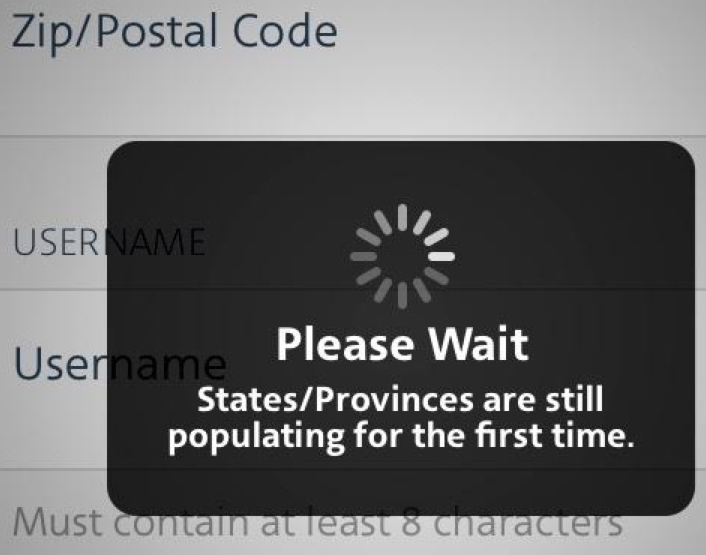
While trying to enter my address into American Airlines' horribly designed phone app, I was asked to wait, because "States/Provinces are still populating for the first time".
What the hell was going on? I'm sure you regular readers will be able to guess.
Read the rest of this entry »
Permalink
August 9, 2016 @ 5:06 am· Filed by Mark Liberman under Nerdview, Semantics
From Bill Benzon:

"Flaming balls" and "reports" may very well be the standard technical terminology for the visual and auditory design features of roman candles. None of the rest of the visible text shows signs of translation problems. But still…
Permalink






